By Michael Kanaabi
The first-half of 2021 has been a tough time across the globe as the resurgence of Covid-19 has taken another turn at devastating lives.
As of Sunday August 8, 2021, the Ministry of Heath reported a cumulative total infection of 94,904 persons, with the numbers still rising.
Locally, the second wave of Covid-19 started to make news towards end of April, picking momentum in May and reaching its peak mid-June with official statistics from the Ministry of Health showing over 1,000 new daily infections in June and deaths rising to over 50 a day.
All this came with lots of uncertainties and panic, especially with in our largely ill-equipped health system to manage the growing number of patients.
The mad rush for oxygen around the country, the inadequate Intensive Care Units (ICU) and High Dependency unit beds, the misappropriation of funds, the discovery of possible remedies have been some of the big headlines locally as the pandemic bites far and wide.
Amidst all these, however, medical personnel, being the frontliners in the fight against the deadly Covid-19, are the most affected group of professionals as they confront this deadly sickness every day in hospitals.
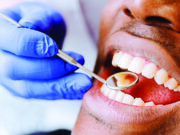
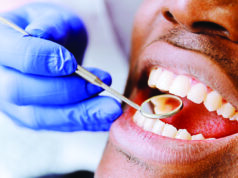
May Namata, a lead laboratory technologist at Women’s Hospital International and Fertility Centre (WHI&FC) in Bukoto, says their workload has gone up tremendously during this period. Namata says they have had to add on Covid-19 tests as well especially for the patients going to be admitted or those they are likely to interface with regularly.
“Unlike a number of lab procedures and tests that would go with the picking blood samples from patients, Covid-19 requires a different type of tests and equipment which has added onto our workload and made everything more cumbersome,” says Namata.
“Our risks on the job have also shot up tremendously.”

She adds: “In our professional training, they always told us how our jobs were high risk with a possibility of infections from samples and as we carry out testing procedures.”
Namata says that she has seen some of their colleagues go down with Covid-19 while some patients they interacted with passed on suddenly. Thereby forcing some people to abandon their jobs.
Dr Joseph Kafuuma, a medical officer at WHI&FC, says transport constraints have greatly brought down patient numbers which in turn brings a down turn in revenue as well for the institution.
Hospital administrators have also had their fair share of ups and downs resulting from the onset of the Covid-19 pandemic and subsequent lockdowns.
Samuel Tamale Sali, one of the directors of the hospital, says: “It has been a logistical nightmare adjusting schedules and arranging transport for staff since the lockdown took shape”.
Other sticking issues emerging out of the pandemic and lockdown, according to Sali, include the cost of oxygen going up abruptly, some consultants charging higher fees for patients attended to and the higher transport costs for staff that have greatly affected proper budgeting and costing for the hospital.
Precautions
One of the precautions Dr Kafuuma says they have undertaken is to cut down on staff numbers within various departments.
“In situations where a department had about five staff working concurrently we have cut this number to two, to reduce chances of exposure and transmission among staff but also due to reduced number of patients being worked on,” he says.
The typical work week has also been reduced from five to three working days for a number of staff as well.
Some staff have also had to isolate for some time after testing Covid- 19 positive.
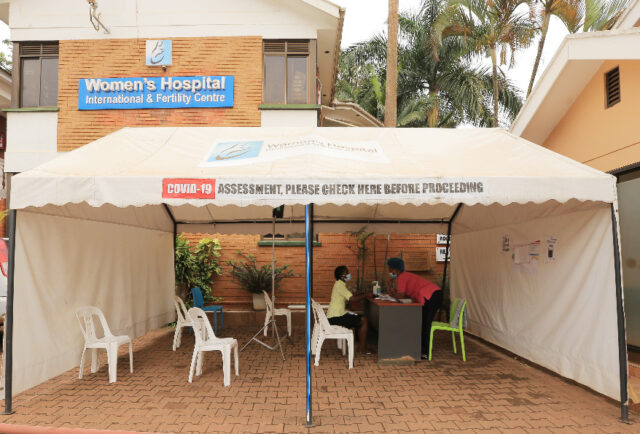
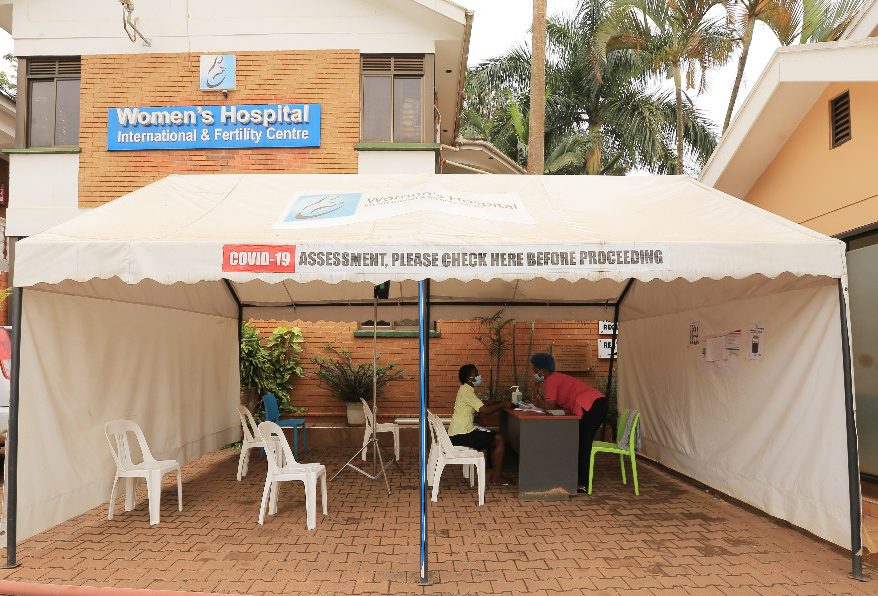
Dr Kafuuma also adds that a decongestion plan has also been implemented at the hospital, starting with reducing staff numbers and erecting tents with in the hospital premises where patients wait for services while observing social distance.
For admitted patients and those receiving antenatal care services from the hospital regularly, mandatory testing for Covid-19 is done besides ensuring all other standard operating procedures (SOPs).
“We have also resorted to attending to patients through modern platforms like Zoom where a physical examination is not required. Our director Dr Tamale Sali has taken the lead in this as it reduces human contact and chances of Covid-19 transmission while the patient still gets the much needed service. However when there is need for further investigation, a travel permit is availed to the patient to come to the hospital,” Kafuuma says.

Administratively, Samuel Sali says the hospital has ensured staff get access to Covid-19 vaccination promptly and also regular and free testing services whenever they feel unwell.
“Adjustments are also continuously being undertaken in terms of scheduling work and transport routines so as to make sure staff are not completely inconvenienced while work also goes on smoothly at the hospital,” he says.
Namata says her employers have provided adequate personal protective equipment for her to do her job effectively in spite of the new challenges and fears they are faced with.
Namata says she takes extra safety measures like sanitizing her workplace four times a day and cleaning all work surfaces after a patient has left, something she was only doing once a day previously.
“At home I have to remove all clothes on arrival and take a full shower before I interact with the rest,” Namata says.
She adds that patients have generally adhered to observing the SOPs.
Recommendations
On what government needs to do going forward to ease the huge burden on private health care providers which has been created by the pandemic and worsened by the lockdown, Dr Kafuuma advises a tax cut on private hospitals as expenses are getting higher while revenues are down due to low numbers in their case.
To the general public, strict adherence to SOPs to protect themselves and getting vaccinated for those who feel it is right should be done to ensure they have a good chance to beat the disease if they get infected.
Sali is positive about the proposed interventions by the Ministry of Health.
However, he emphasises that they should be more effective and vigilant when it comes to implementation of the interventions to manage the pandemic.
Namata says medical professionals who are on the frontline of fighting this pandemic should get a pay raise and risk allowances to keep them motivated.
She also suggests the government should make personal protective equipment affordable so as to keep the medics safe and also keep the cost of working on patients affordable.
“Strong top-down intervention, both policy wise and in implementation, should be conducted to stop greedy profit-seeking business people from hiking the cost of gloves and masks plus other equipment we use in hospitals,” Namata says.
She concludes that the government should cut the cost of Covid-19 tests to ensure it is affordable for the common people to encourage faster mass testing, detection and management of the disease.