By Sarah Achen
October is breast cancer awareness month, but also serves as a reminder of the importance of vaccines.
Many people around the globe remain hesitant about vaccination. But amidst such, many vaccines have been developed, tried and successfully used over the years to prevention various diseases.
In Uganda, for instance, polio vaccination brought to an end polio cases following government’s campaign to “Kick polio out of Uganda” in the 1990s and early 2000s. Only recently did the country register a few cases again.
According to information published on cancer.net, vaccines can prevent healthy people from getting certain cancers caused by viruses. For instance, vaccines for chicken pox or flu protect the body against the causal viruses.
However, this type of vaccines only work if a person is vaccinated before they are infected with the virus.
There are two types of cancer vaccines approved by the U.S Food and Agricultural Administration (FDA):
HPV vaccine: This protects people against human papillomavirus (HPV).
If this virus stays in the body for a long time, it can cause some types of cancer.
The FDA has approved HPV vaccines to prevent cervical, vaginal, and vulvar cancers.
Hepatitis B vaccine: This protects people against hepatitis B virus (HBV). This virus can cause liver cancer.
Medical researchers are working to advance human understanding of how to prevent, detect, and treat breast cancer.
They are also looking at how to address disparities and improve quality of life for survivors of the disease.
Breast cancer awareness
The October breast cancer awareness month is an annual campaign to observe and raise awareness about breast cancer, the second most common cancer among women in Uganda.
According to Uganda Cancer Institute’s Public Relations Officer, Ms Christine Namulindwa, current trends indicate that by 2030, cancer cases will be increasing by 48.4 per 100,000 women, with an expected 1,310 new cases between 2026 and 2030.
A 2021 Global Cancer Observatory report reveals that new breast cancer cases in Uganda stand at 2,375; about eight per cent of all cancers in the country.
So far, there is no vaccine in place for prevention of breast cancer.

Symptoms
Namulindwa says symptoms of breast cancer include breast lump or thickening that feels different from the surrounding tissues and change in the size, shape or appearance of the breast.
Others also include: peeling, scaling, crusting or flaking of the breast skin or pigmented area of skin surrounding the nipple, and redness or pitting of the skin over the breast like that of an orange.
She says common risks for this type of cancer are: being female, increasing age, family/personal history of breast cancer conditions, inherited genes that increase cancer risk, obesity, radiation exposure and alcohol use.
Uganda has a breast cancer age-standardized incidence and mortality rate standing at 21.3 per 100,000 population and 10.3 per 100,000 population respectively.
New hope for patients
According to a recent BBC report, scientists in the UK have revealed that a new type of cancer therapy using a common virus to infect and destroy harmful cells is showing promising results in its early stage of human trials.
“One patient’s cancer vanished, while others saw their tumours shrink,” the report reads in part.
The drug is a weakened form of the cold sore virus (herpes simplex) that has been modified to kill tumours.
About 40 patients have tried the treatment as part of the trial. Some were given the RP2 virus injection alone, while others received a combination of RP2 and nivolumab, a cancer treatment drug.
Three out of nine recipients of the RP2 saw their tumours shrink. While seven out of 30 who got the combined treatment are reportedly benefitting also.
The report further reveal that side effects such as tiredness were generally mild.
Larger and longer studies shall be needed, but experts say the injection might ultimately offer a lifeline to more people with advanced cancers.
Benefits
Dr Sabrina Kitaka, a senior lecturer, Paediatrics and Child Health at Makerere University, says when a pathogen infects the human body, its defense (immune system) are automatically triggered. These attack the pathogen and destroy or overcome it.
Vaccines contain weakened or inactive parts of a particular organism (antigen) that triggers an immune response within the body.
However, newer vaccines contain the blueprint for producing antigens rather than the antigen itself.
“Regardless of whether the vaccine is made up of the antigen itself or the blueprint so that the body will produce the antigen, this weakened version will not cause the disease in the person receiving the vaccine, but it will prompt their immune system to respond as much as it would have on its first reaction to the actual pathogen,” Dr Kitaka says.
Some vaccines require multiple doses, given weeks or months apart.
This is sometimes needed to allow for the production of long-lived antibodies and the development of memory cells.
In this way, the body is trained to fight the specific disease-causing organism, building up the memory of the pathogen so as to rapidly fight it if and when exposed in the future.
Vaccination protects the vaccinated persons and those around them who may be vulnerable to the diseases, thereby reducing the risk of diseases spreading among family members, school mates, work colleagues, friends and neighbours, among others.
Dr Kitaka says when enough people in a population are immune to an infectious disease, the disease is unlikely to spread from person-to-person.
Consequently, vaccines indirectly protect vulnerable community members such as babies, the elderly, people with weak immune systems, cancer patients, and other groups that cannot be vaccinated for medical reasons.
Dr Anthony Male of Health Choice Centre in Mukono, says to ensure community immunity against diseases like measles, public health authorities recommend that at least 95 per cent of the population gets vaccinated against the disease with two doses of the vaccine (the MMR vaccine, which protects against measles, mumps and rubella).
However, people cannot rely on community immunity for some infectious diseases.
For example, tetanus can be encountered due to common injuries, including dog or cat bites.
This makes vaccination the only way to ensure direct protection against tetanus.
Besides, vaccination also reduces the social, psychological and financial burdens of diseases on people and governments, thereby, reducing pressure on social and healthcare systems.
Side effects
It is common for people to experience changes such as body pain, headache, tiredness, swelling, and redness on the arm where the shot was given, after getting vaccinated.
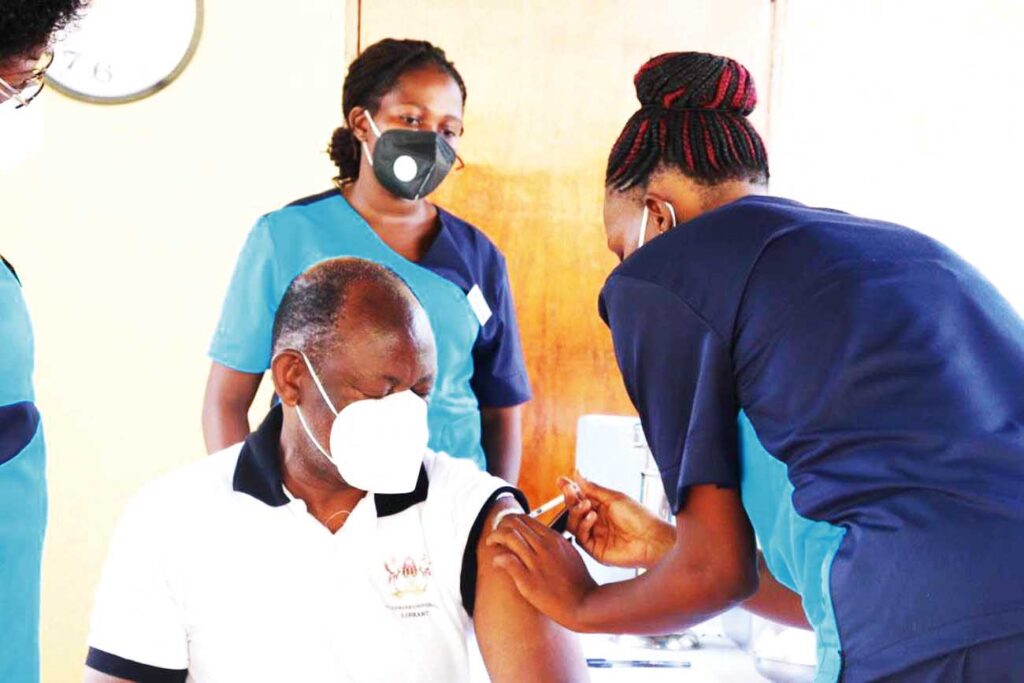
Vaccine coverage
According to the commissioner in charge of reproductive health at the Ministry of Health, Dr Jesca Nsungwa, there is no specific sum of Ugandans vaccinated against the various diseases so far.
Nsungwa says this is so because the number keeps changing as new people continue to get the jabs.
“Vaccines target different categories of people starting from children in schools,” Nsungwa says, “We are addressing the out-of-school young people as we continue with surveillance.”
According to Nsungwa, there are more than 10 new vaccines on board now.
She says this year, the ministry went beyond targets in both first and second doses of the Covid-19 vaccine.
The platform is expanding from vaccines such as yellow fever, pneumonia and typhoid, among others.
Nsungwa says the ministry is using various social media platforms to disseminate information on the need for every Ugandan to embrace vaccines.
She says district health teams also facilitated dialogues with health workers to hear their concerns and address their fears about vaccines.
The ministry encourages mothers and parents to demand for vaccines at health facilities near them.
There have been training opportunities for health workers to give correct information to parents and young girls on available services at their facilities.
In the case of HPV vaccine, the health workers involve family members of girl children prior to vaccinating them. The HPV vaccine is taken by girls and women between 9 and 25 years.
Myths about vaccines

I remember when I was young, my parents and I feared vaccines.
People used to say they make one impotent, barren and lame.
But it was the same vaccines that helped us to grow into healthy adults.
So, much as the government has done a lot, it needs to do more than just sending constant reminders on the importance of vaccines.

Vaccines are good when they are not expired. Ugandans do not embrace vaccines because government has not done a lot of sensitisation to change the negative attitude.
I have heard things like vaccines are meant to reduce our life span. That is the reason I have not yet taken the Covid-19 vaccine.
With time, I may change my mind and go for it because even my mother got it and she is still alive and healthy.

I feared the Covid-19 vaccines and all other types of vaccines because people said they contained harmful chemicals.
As I interrogated further, I discovered that everybody is entitled to their view and that the choice to take the vaccine was entirely mine because it concerned my life.
My aunt once lost a baby because she was against vaccines. But after talking to a health expert, she was told that most people who react negatively to vaccines are those with underlining conditions, but they wrongly blame the vaccines.